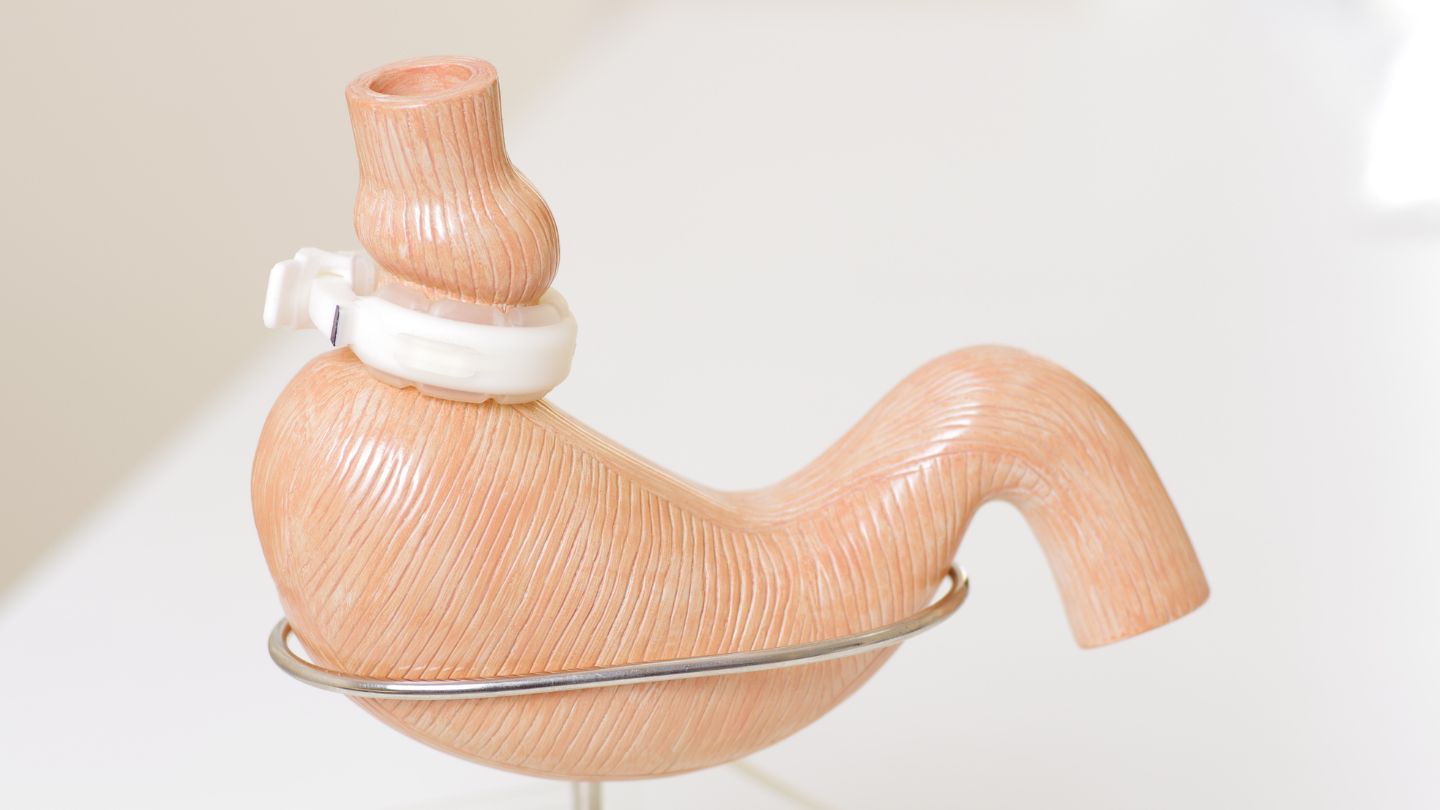
How Do Thyroid Issue Affect Weight loss After Bariatric Surgery
Bariatric surgery is a life-changing procedure that helps many people achieve significant weight loss and improved health. However, for some, losing weight after surgery can be more challenging than expected, and underlying thyroid issues might be the reason. Thyroid problems can affect metabolism, energy levels, and overall weight loss progress. In this blog, we’ll explore how thyroid conditions impact weight loss after bariatric surgery and what you can do to manage these challenges effectively.
Key Takeaways
- Thyroid dysfunction, such as hypothyroidism and hyperthyroidism, can significantly hinder weight loss efforts, particularly in obese individuals, emphasizing the need for early diagnosis and management.
- Bariatric surgery is effective in improving thyroid hormone levels, with many patients experiencing reduced TSH levels and improved thyroid function post-surgery, aiding in their overall weight loss journey.
- Managing thyroid health before and after bariatric surgery is essential for minimizing complications and enhancing weight loss outcomes, necessitating regular monitoring and possible adjustments in thyroid hormone replacement therapy.
Understanding Thyroid Function
The thyroid gland, a diminutive structure with the shape of a butterfly situated at the neck’s base, has a critical role in controlling various vital bodily operations. This organ is responsible for producing hormones that are essential for regulating metabolism, energy provision, and even body weight. Maintaining normal thyroid function is crucial as it affects numerous physiological aspects such as heart rate, respiration rate, body temperature control, and cholesterol management.
Hormones produced by the thyroid gland, like thyroxine (T4) and triiodothyronine (T3), have key roles in dictating energy usage and dietary consumption through their influence on carbohydrate and fat metabolism. Ensuring proper levels of these hormones means maintaining an equilibrium of receptors within the system necessary to balance metabolic processes, including both thyroid and other thyroid hormones.
Nevertheless, when there’s an imbalance in how the thyroid functions (with conditions such as hypothyroidism, which involves reduced activity, or hyperthyroidism, where excessive hormone production occurs), individuals may face challenges related to weight control, those suffering from hypothyroidism frequently struggle with an unanticipated weight increase along with difficulties in shedding pounds due to hormonal disturbances.
In those who are obese, specifically higher TSH figures alongside altered levels of relevant hormones might suggest potential issues concerning thyroid health. Deficiencies in iodine – crucial for the synthesis of these regulators – can Complicate metabolic rates, leading to complications regarding one’s mass profiles. Understanding this complex relationship allows better development strategies aimed at managing weights effectively amongst people contending obesity intertwined with concerns surrounding their thyroids.
Thyroid Dysfunction and Obesity

The complex connection between obesity and thyroid dysfunction forms a problematic loop. Studies have indicated that the risk of developing hypothyroidism is nearly twice as high in obese individuals compared to those who are not overweight, with an increased rate of overt hypothyroidism hampering their ability to lose weight.
A significant hurdle presents itself when many patients experiencing mild deficiencies in thyroid hormone go unrecognized due to concurrent issues with obesity. This condition can affect thyroid function while conversely. Disturbances within the gland can lead to excess weight, forging a two-way relationship. In cases where elevated levels of thyroid-stimulating hormones are observed among obese persons, it could signify underlying problems with the gland that must be addressed for effective regulation of body mass through interventions such as heightened serum TSH concentrations.
When considering autoimmune diseases affecting this endocrine organ, like Hashimoto’s disease, these conditions may exacerbate struggles related to controlling one’s body weight in people dealing with excessive fat accumulation. The link highlights why comprehensive screening for disorders impacting this system is necessary, given its prevalence among heavily overweight subjects.
Disorders stemming from hormonal imbalances caused by suboptimal functioning glands often result in difficulty shedding pounds even amid dietary changes and physical activity regimens—underlining how critical resolving endocrine disruptions is when devising strategies targeting substantial fat reduction for affected individuals.
Those struggling with severe or morbidly heavy weights should pay particular attention since correcting any malfunction early enhances opportunities both for successful slimming down and improved management across all aspects regarding wellbeing—a vital consideration before opting into bariatric procedures aimed at overcoming challenges associated with considerable girth.
Effects of Bariatric Surgery on Thyroid Hormones
The effects of bariatric surgery on weight loss are substantial, particularly with respect to thyroid hormones. After such surgical procedures, levels of the thyroid stimulating hormone (TSH) significantly decrease. This decline is more strongly associated with initial TSH values rather than subsequent changes in body mass index (BMI), underscoring its significance as a component of the metabolic transformations spurred by weight reduction operations.
Roux-en-Y gastric bypass has been specifically shown to cause considerable drops in fasting TSH levels following the procedure, suggesting an enhancement in thyroid function. Notably, none of the patients transitioned into overt hypothyroidism post-surgery, which attests to its benign influence on thyroid health.
Procedures like Roux-en-Y gastric and laparoscopic sleeve gastrectomy have observable positive impacts on levels of thyroid hormones. Studies reveal notable decreases in both BMI and TSH at 6-month and 12-month intervals after undergoing surgery while maintaining stable free thyroxine (T4) levels. This suggests that these surgeries support not only weight reduction but also facilitate consistent regulation of thyroid function.
For obese patients who maintain normal euthyroid status but possess slightly elevated TSH concentrations, significant reductions were observed following their bariatric operations. An impressive 89.5% saw resolution from subclinical hypothyroidism one year after having a Roux-en-Y gastric bypass done—a fact that spotlights the advantageous influences that such interventions can have on those battling obesity-related issues within their endocrine systems.
This information sheds light on potential advantages related to improving one’s conditions relating to overall health when considering options for managing excessive weight through bariatric intervention—specifically regarding enhancing outcomes concerning both effective management of body weight and promoting general well-being through better-regulated functioning within the realm governed by crucially important secretions like those produced by our own bodies’ glands responsible for metabolism: namely improved effectiveness via targeted therapies addressing overweight individuals’ concerns involving their respective rates or capacities pertaining toward proper physiological utilization/utilities drawing upon substances known simply as ‘thyroid hormones.’
Read more: Gastric Bypass Surgery vs. Gastric SleeveWeight Loss Outcomes in Patients with Thyroid Issues
Bariatric surgery is the most effective treatment for obesity in an obese patient with thyroid abnormalities. Weight loss outcomes can vary significantly among patients with different thyroid conditions. Some patients experience remarkable weight loss, while others see more modest results.
A critical factor influencing weight loss outcomes is the reduction in thyroid-stimulating hormone (TSH) levels post-surgery. Significant weight loss progressively decreases TSH levels, which is closely associated with the extent of weight loss over time. This correlation suggests successful weight loss efforts can positively impact thyroid function.
Preoperative excessive body mass index (BMI) loss is significantly linked to lower TSH values post-bariatric surgery. Patients who lose body weight before surgery are more likely to see post-surgery improvements in thyroid function. Post-surgery changes in TSH levels often tie more closely to weight loss efforts than the surgical procedure itself.
Patients with morbid obesity typically have elevated TSH levels compared to healthy individuals before surgery. These imbalances can affect the extent of weight loss in patients undergoing bariatric surgery. For some, significant weight loss may reduce the need for thyroid hormone replacement therapy. One year post-bariatric surgery, 13.2% of participants diagnosed with hypothyroidism no longer required hormone replacement therapy.
These outcomes help patients set realistic expectations and highlight the importance of managing thyroid health for successful weight loss. Addressing thyroid issues and optimizing hormone levels improves the chances of achieving lasting weight loss results.
Read more: Top Questions to Ask Your Weight Loss Surgeon Before Surgery
Managing Thyroid Problems Before and After Surgery

Managing thyroid problems before and after bariatric surgery is crucial for minimizing complications and enhancing weight loss outcomes. Optimizing thyroid hormone levels before surgery reduces the risk of perioperative complications. Patients with known thyroid disorders should undergo a TSH test as part of their preoperative assessment for optimal treatment.
Addressing thyroid issues before surgery is critical for patients. Many hypothyroid patients undergoing bariatric surgery may continue to require thyroid hormone replacement therapy but at a lower dosage one-year post-procedure. Bariatric surgery benefits thyroid function, especially in hypothyroid patients who may require reduced doses of thyroid hormone replacement therapy post-surgery.
Thyroid hormone replacement therapy should be adjusted based on circulating thyrotropin levels and individual clinical data for optimal outcomes. Postoperative management of thyroid hormone levels is essential to avoid complications like myxedema coma, a severe form of hypothyroidism. Routine preoperative thyroid disease screening is not recommended unless the patient is symptomatic.
Patients with thyroid disorders often experience significant mood swings and energy level fluctuations, impacting their readiness for bariatric surgery. Individuals with thyroid issues should be aware of their emotional state and seek mental health support before undergoing bariatric surgery. Effective thyroid problem management improves overall health and increases the chances of successful weight loss.
Emotional and Psychological Effects
Issues with the thyroid can have a significant impact on one’s emotional and psychological health, affecting every aspect of their lives. Those who suffer from thyroid disorders often experience mood swings and variations in energy levels. Such changes can disrupt personal relationships, social activities, and professional responsibilities, making it difficult to maintain consistency and productivity.
For individuals undergoing bariatric surgery treatment for weight loss, managing these mood fluctuations becomes especially challenging when also contending with regulating the thyroid. The emotional roller coaster may weaken their resolve and dedication to shed pounds, underlining the necessity of addressing such concerns during this period.
It is essential that patients acknowledge any emotional difficulties they encounter as part of preparation for bariatric surgery—promptly seeking mental health support if necessary. Access to psychological assistance is vital in navigating through emotions effectively while keeping sights set firmly on achieving weight loss objectives. Tackling both emotional and psychological hurdles associated with thyroid complications can lead not only to enhanced overall well-being but also bolster the likelihood of success in their journey toward weight reduction.
Read more: Most Common Bariatric Surgery MythsSummary
Thyroid issues can significantly impact weight loss after bariatric surgery, making it critical to address thyroid health as part of the weight management process. By understanding and managing thyroid function, individuals can enhance the effectiveness of bariatric procedures, achieve better hormonal balance, and work towards sustainable, long-term results.
At Wellstar Comprehensive Bariatric Services, we take a holistic approach to your weight loss journey. Our team is dedicated to addressing all aspects of your health, including thyroid function, to ensure successful outcomes. We offer expert weight loss surgery in Austell and surrounding areas such as Smryna, Cobb, LaGrange, West GA, and Marietta. Contact us today to learn how we can support your transformation and help you achieve lasting success.
Frequently Asked Questions
How does thyroid dysfunction affect weight loss after bariatric surgery?
Thyroid dysfunction significantly hinders weight loss after bariatric surgery due to hormonal imbalances that may promote weight gain.
It is essential to manage thyroid health to achieve optimal weight loss results.
What is the impact of bariatric surgery on thyroid hormone levels?
Bariatric surgery significantly decreases thyroid-stimulating hormone (TSH) levels, primarily correlating with initial TSH values rather than changes in body mass index (BMI).
This reduction reflects important metabolic changes associated with the surgery.
How can patients manage their thyroid problems before undergoing bariatric surgery?
Patients should ensure optimal management of their thyroid disorders by undergoing a TSH test prior to bariatric surgery.
Addressing and stabilizing hormone levels beforehand is crucial for minimizing complications and improving weight loss results.
What are the emotional and psychological effects of thyroid issues during weight loss treatment?
Thyroid issues significantly affect emotional and psychological well-being, leading to mood swings and altered energy levels that can disrupt personal and professional life.
Therefore, seeking mental health support is essential for effectively managing these challenges during weight loss treatment.