The Effect of Smoking on GERD and Acid Reflux: What You Need to Know
Looking to understand the effect of smoking on GERD and acid reflux? Smoking can worsen these conditions by weakening the lower esophageal sphincter and increasing stomach acid production. This blog explores how smoking impacts GERD and acid reflux symptoms and the benefits of quitting.
Key Takeaways
- Cigarette smoking significantly exacerbates GERD by increasing stomach acid production and impairing the function of the lower esophageal sphincter (LES), which allows acid to enter the esophagus.
- Quitting smoking leads to a marked reduction in GERD symptoms and improves overall health-related quality of life, emphasizing the need for smoking cessation in GERD management.
- Lifestyle modifications, including dietary adjustments and weight management, alongside smoking cessation, are essential for effectively managing GERD and preventing complications.
Understanding GERD and Acid Reflux
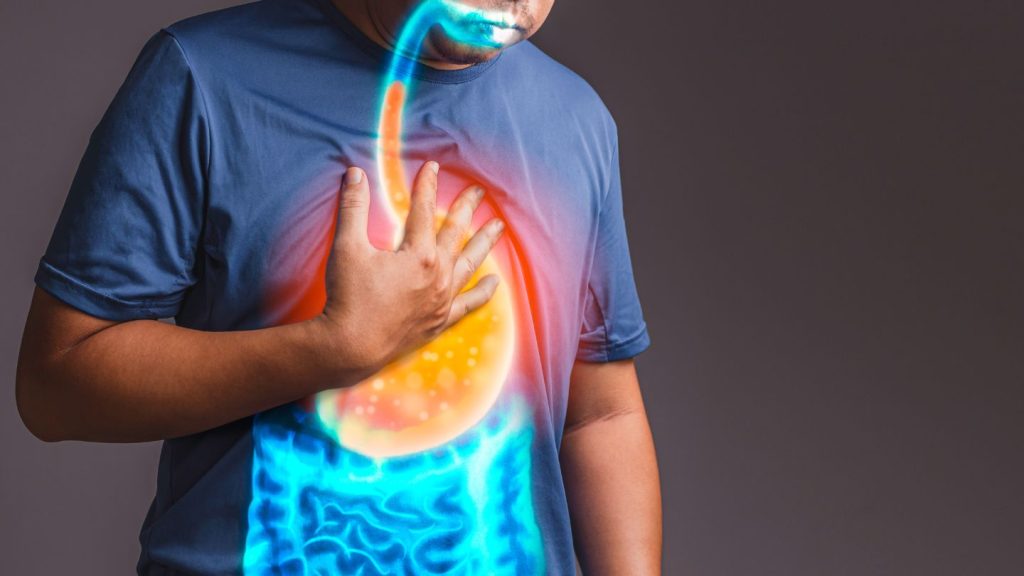
Gastroesophageal reflux disease (GERD), which is commonly known as acid reflux, is a widespread digestive disorder that affects countless individuals around the globe. This condition manifests when stomach acid regularly reverses its course into the esophagus—the conduit between your mouth and stomach—resulting in potential inflammation of the esophageal lining and resulting in discomfort along with various other symptoms. The term gastro-oesophageal reflux disease refers to this same set of problems.
The processes involved in acid reflux are intricate and involve several components, such as the lower esophageal sphincter (LES), stomach acid, and intra-abdominal pressure. Acidic contents from the stomach can make their way back up into the esophagus if there’s an abnormal weakening or relaxation of LES—a muscular valve situated where your esophagus concludes—thereby leading to irritation and damage within.
Left unmanaged, this illness holds potential consequences for different body parts, including implications for respiratory pathways like windpipe involvement, possibly escalating to more critical health complications.
GERD Symptoms
Gastroesophageal reflux disease (GERD) is recognized by a variety of symptoms that can significantly affect comfort and well-being. Frequent heartburn, characterized by a sharp burning sensation in the chest, which may extend to the throat, is among the most prevalent signs. This pain typically intensifies post-meal or during recumbent positions and has the potential to be so intense that it’s mistaken for cardiac arrest.
Symptoms such as acid regurgitation also play a prominent role in this condition. Stomach acid or bile reverses its course back into the esophagus, leaving an unpleasant sour or bitter aftertaste. Sufferers might contend with chest discomfort, challenges swallowing food effectively, and persistent coughing fits. These enduring episodes of heartburn, along with related manifestations, often point towards gastroesophageal reflux disease (GERD).
Causes of Acid Reflux
A variety of elements can lead to the onset of acid reflux, with malfunctioning of the lower esophageal sphincter (LES) at its core. This valve-like structure’s main role is to contain stomach acid by sealing it within the stomach. If it becomes weak or relaxes when it shouldn’t, this barrier fails. Consequently, this permits the escape of stomach acid into the esophagus and triggers episodes of reflux.
Additional factors that may incite such events include a rise in intra-abdominal pressure, which can force contents from the stomach back up into the esophagus. Such pressures might stem from conditions like obesity or pregnancy, as well as certain food items and drinks known for causing LES relaxation.
Recognizing these contributing agents is key in formulating effective interventions aimed at alleviating symptoms associated with acid reflux and enhancing overall gut health.
The Link Between Smoking and GERD
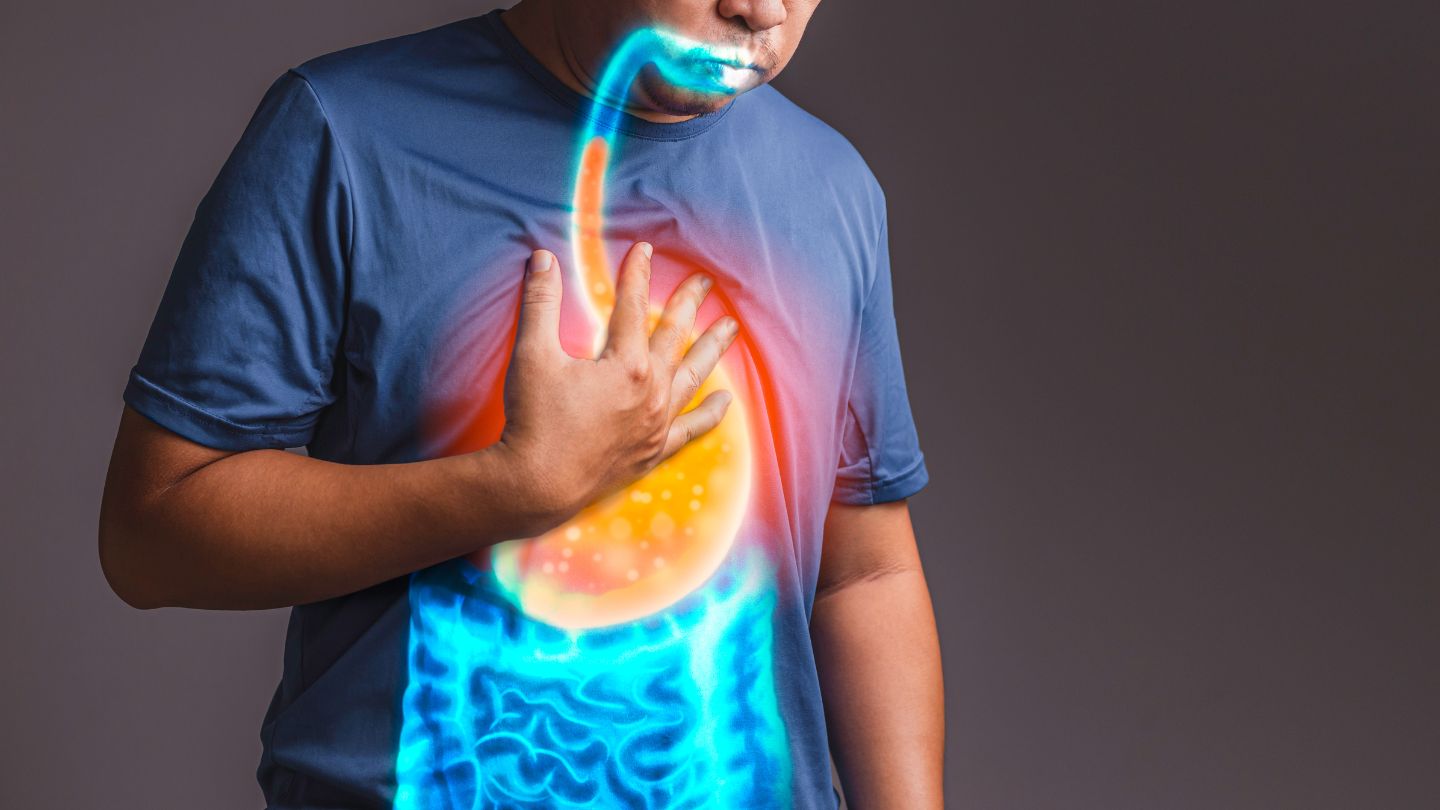
Cigarette smoking significantly contributes to the onset and worsening of gastroesophageal reflux disease (GERD). Research has consistently found that smokers have a higher likelihood of suffering from GERD because smoking boosts stomach acid production, weakens the lower esophageal sphincter’s functionality, and diminishes the esophagus’s capacity for acid clearance.
Beyond its detrimental effects on lung health, cigarette smoke also adversely affects the digestive system. In those diagnosed with GERD, continued smoking can exacerbate symptoms and compromise treatment outcomes. Healthcare professionals strongly recommend that individuals with this reflux disease quit smoking in order to enhance their symptom management and overall well-being.
Impact on Lower Esophageal Sphincter
Smoking intensifies GERD symptoms by impairing the function of the lower esophageal sphincter (LES). Nicotine and other substances in tobacco smoke reduce LES pressure, making it easier for stomach contents to escape into the esophagus. In addition to relaxing the LES, smoking interferes with esophageal motility, slowing down the natural clearance of acid from the esophagus and allowing prolonged exposure to harmful gastric contents.
This dual effect—reduced LES tone and delayed acid clearance—creates a cycle of irritation and inflammation that can make GERD more persistent and harder to manage. Medical professionals often address these issues through a combination of targeted therapies, lifestyle counseling, and sometimes surgical interventions, especially when lifestyle changes alone are not effective.
Increased Stomach Acid Production
Smoking stimulates the production of gastric acid, further intensifying GERD symptoms. Substances in cigarette smoke activate acid-secreting cells in the stomach, resulting in an overly acidic environment. When paired with an already weakened LES, this excess acid easily finds its way into the esophagus, leading to increased discomfort and potential mucosal damage.
Gastroenterologists often address this concern with tailored medical treatments like acid suppression therapy and comprehensive evaluation of each patient’s triggers and symptom patterns. It is important for individuals experiencing chronic reflux to seek professional care rather than relying on over-the-counter remedies, which may not address the root cause.
Impaired Esophageal Acid Clearance
Efficient clearance of acid in the esophagus is essential for GERD symptom control, yet smoking significantly hampers this process. Smoking reduces saliva production and impairs the effectiveness of bicarbonate—an essential acid-neutralizing agent. The result is a slower neutralization of acid that enters the esophagus, allowing prolonged irritation and increasing the risk of esophageal damage.
Specialists may recommend diagnostic tools such as esophageal pH monitoring and manometry to evaluate acid clearance efficiency and esophageal function. These tests enable clinicians to develop a treatment plan that is specific to each individual’s condition rather than relying on generic self-care measures.
Smoking Cessation and GERD Improvement

Quitting smoking yields significant improvements in digestive health, particularly for those suffering from GERD. Cessation helps restore the normal function of the lower esophageal sphincter, reduces acid production, and enhances the esophagus’s ability to clear acid effectively. Together, these changes contribute to a noticeable decrease in GERD symptoms.
In a study assessing symptom improvement, 43.9% of former smokers experienced relief from GERD symptoms, compared to only 18.2% of current smokers. These numbers highlight the importance of incorporating smoking cessation into a professional care plan for GERD. Healthcare providers often offer integrated support services such as behavioral therapy, pharmacologic aids, and follow-up evaluations to support long-term success in quitting.
Reduction in GERD Symptoms
A substantial decrease in GERD symptoms has been observed among individuals who have successfully quit smoking. Specifically, 43.9% of those who stopped smoking experienced a reduction in their symptoms, whereas a mere 18.2% of ongoing smokers reported similar improvements. This data underscores the crucial role that quitting smoking plays in managing GERD effectively.
Those participants who gave up smoking noted not only a diminished frequency but also lessened the severity of their GERD symptoms, which consequently led to an enhancement in their health-related quality of life. Such findings emphasize the pivotal importance that making lifestyle alterations—particularly cessation of smoking—has on securing improved health outcomes for sufferers of GERD.
Enhanced Health-Related Quality of Life
The positive effects of smoking cessation extend well beyond digestive relief. Former smokers frequently report improvements in sleep quality, energy levels, and overall physical comfort—areas that are often negatively affected by chronic reflux. Additionally, studies show that individuals who stop smoking experience lower stress levels and reduced dependency on acid-reducing medications over time.
Health professionals emphasize that quality of life improvements are more sustainable when smoking cessation is part of a broader care plan that may include dietary guidance, medication adjustments, and ongoing monitoring to track progress and prevent relapse.
Long-Term Benefits
The long-term benefits of quitting smoking for individuals with GERD include more than just symptom relief—they also involve a decreased risk of complications such as Barrett’s esophagus and esophageal cancer. Smoking contributes to chronic inflammation and cellular changes in the esophageal lining, raising the risk for precancerous conditions. Eliminating tobacco use reduces these risks significantly.
Professional care providers often conduct regular endoscopic screenings for patients with long-standing GERD symptoms and a history of smoking, ensuring early detection and intervention if complications arise. This proactive approach underscores the importance of long-term clinical support in maintaining gastrointestinal health.
Risk Factors and Lifestyle Changes

Numerous factors related to one’s lifestyle, such as dietary habits and tobacco use, can markedly aggravate the symptoms of GERD. The habit of smoking notably constitutes a considerable risk factor for the onset of GERD since it not only weakens the lower esophageal sphincter (LES) but also boosts stomach acid production. Having a higher body mass index (BMI) is associated with increased abdominal pressure, which may lead to acid reflux.
For effective management of GERD, tackling these risk factors via lifestyle modifications is crucial. This involves giving up smoking and altering eating patterns, along with integrating medical treatments into an all-encompassing strategy aimed at enhancing digestive health and alleviating the symptoms associated with GERD.
Body Mass Index (BMI)
Body mass index (BMI) is a key factor in the development and management of GERD. Higher BMI levels increase intra-abdominal pressure, which can push stomach acid upward into the esophagus. Individuals classified as overweight or obese face a significantly higher risk of experiencing reflux-related symptoms.
Professionally supervised weight management programs can help patients achieve a healthier BMI through evidence-based strategies, which may include medical nutrition therapy, behavioral counseling, and, in some cases, bariatric surgery. Unlike at-home diets, these comprehensive programs are tailored to each individual’s needs and are proven to produce more consistent long-term results.
Dietary Adjustments
Diet plays a critical role in managing GERD symptoms, but generalized advice may not work for everyone. While avoiding common triggers like spicy foods, carbonated beverages, and fatty meals is often recommended, the impact of specific foods can vary from person to person.
A registered dietitian or clinical nutritionist can help identify personal dietary triggers through guided elimination diets and structured food tracking. This individualized approach ensures more accurate results and better symptom control than self-directed food experiments, which can often be inconsistent or misleading.
Medical Treatments
Medical treatments for GERD are most effective when tailored to the individual. Options include proton pump inhibitors (PPIs), H2 receptor antagonists, and promotility agents—all prescribed based on a detailed evaluation of symptom severity, frequency, and underlying causes.
Physicians often combine these treatments with lifestyle modifications and regular follow-up assessments to adjust therapy as needed. It is crucial for patients to avoid relying solely on over-the-counter medications or unverified online remedies, as these can mask symptoms without addressing the root problem.
Clinical Evidence and Studies
Numerous investigations have determined that smoking is closely related to the intensification of gastroesophageal reflux disease (GERD) symptoms. Evidence suggests that tobacco use can play a substantial role in both triggering and aggravating the signs of GERD. Conversely, ceasing to smoke over an extended period has been associated with consistent declines in the occurrence of this reflux disease and enhancements in overall gastrointestinal well-being.
Consequently, these insights underscore the importance of quitting smoking as an essential component in controlling GERD. Healthcare experts, along with research scholars, endorse smoking cessation as a vital element within an overarching strategy for mitigating symptoms tied to gastroesophageal reflux and enhancing patients’ life quality.
Study on Smoking Exposure and Reflux Esophagitis
A considerable research effort investigating the association between smoking and reflux esophagitis has found that individuals who currently smoke are significantly more prone to develop this ailment than those who have never smoked. According to the study, active smokers face a 2.4-fold greater risk of experiencing reflux esophagitis when compared with people who have never smoked, while individuals who previously smoked and accumulated more than 20 pack-years of smoking history face a risk increase factor of 2.5.
The correlation between the number of pack-years a person has smoked and their elevated likelihood of developing reflux esophagitis underscores the negative impact smoking can have on one’s gastrointestinal well-being. These results underline how crucial it is for smokers to cease tobacco use in order to lower their chances of encountering serious complications from GERD (gastroesophageal reflux disease).
Long-Term Benefits of Smoking Cessation
It is well-established that quitting smoking has long-term advantages for both GERD management and the overall health-related quality of life. In a study evaluating these benefits, participants’ reflux symptoms, their general health-related quality of life, and their success in smoking cessation were examined through self-reported questionnaires. The primary measurements taken into account included the occurrence rate of GERD, symptom frequency, and scores pertaining to related quality of life.
The findings indicated substantial enhancements in GERD symptoms as well as an overall increase in health-related quality among individuals who successfully ceased smoking. These outcomes emphasize the critical role that quitting tobacco plays within a holistic strategy focused on controlling GERD while simultaneously promoting enduring health improvements.
Summary
The connection between smoking and GERD is well-documented, with smoking intensifying GERD symptoms by weakening the lower esophageal sphincter, boosting acid production, and hindering acid clearance. Quitting smoking not only alleviates these symptoms but also decreases the risk of long-term complications and improves overall quality of life.
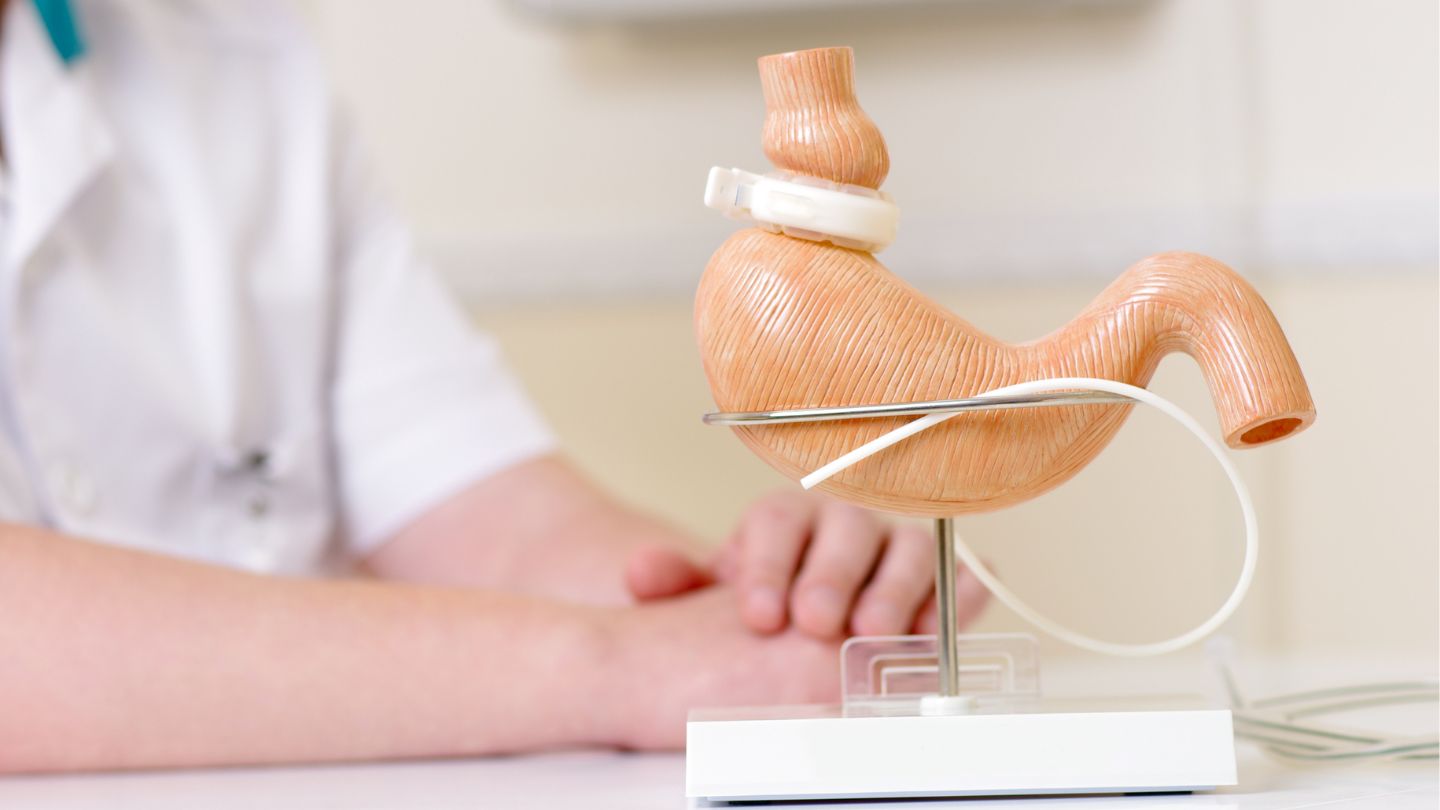
At Wellstar Comprehensive Bariatric Services, we recognize the intricate relationship between weight, lifestyle habits, and digestive health. Our multidisciplinary team provides tailored care plans for effective GERD treatment in Marietta, Smryna, Cobb, Austell, LaGrange, and West GA, incorporating evidence-based interventions such as weight loss strategies, nutritional guidance, and long-term support. If you are experiencing persistent GERD symptoms and are ready to explore lasting solutions, contact us to achieve better health.
Frequently Asked Questions
1. Can quitting smoking improve acid reflux even without other lifestyle changes?
Yes, studies show that stopping smoking alone can significantly reduce acid reflux symptoms, even without major dietary or weight changes.
2. Why does smoking affect acid clearance in the esophagus?
Smoking reduces saliva production and bicarbonate levels, which are both essential for neutralizing and clearing acid from the esophagus.
3. How long after quitting smoking might GERD symptoms improve?
Many people notice symptom relief within a few weeks, but full improvement may take several months, depending on individual health factors.