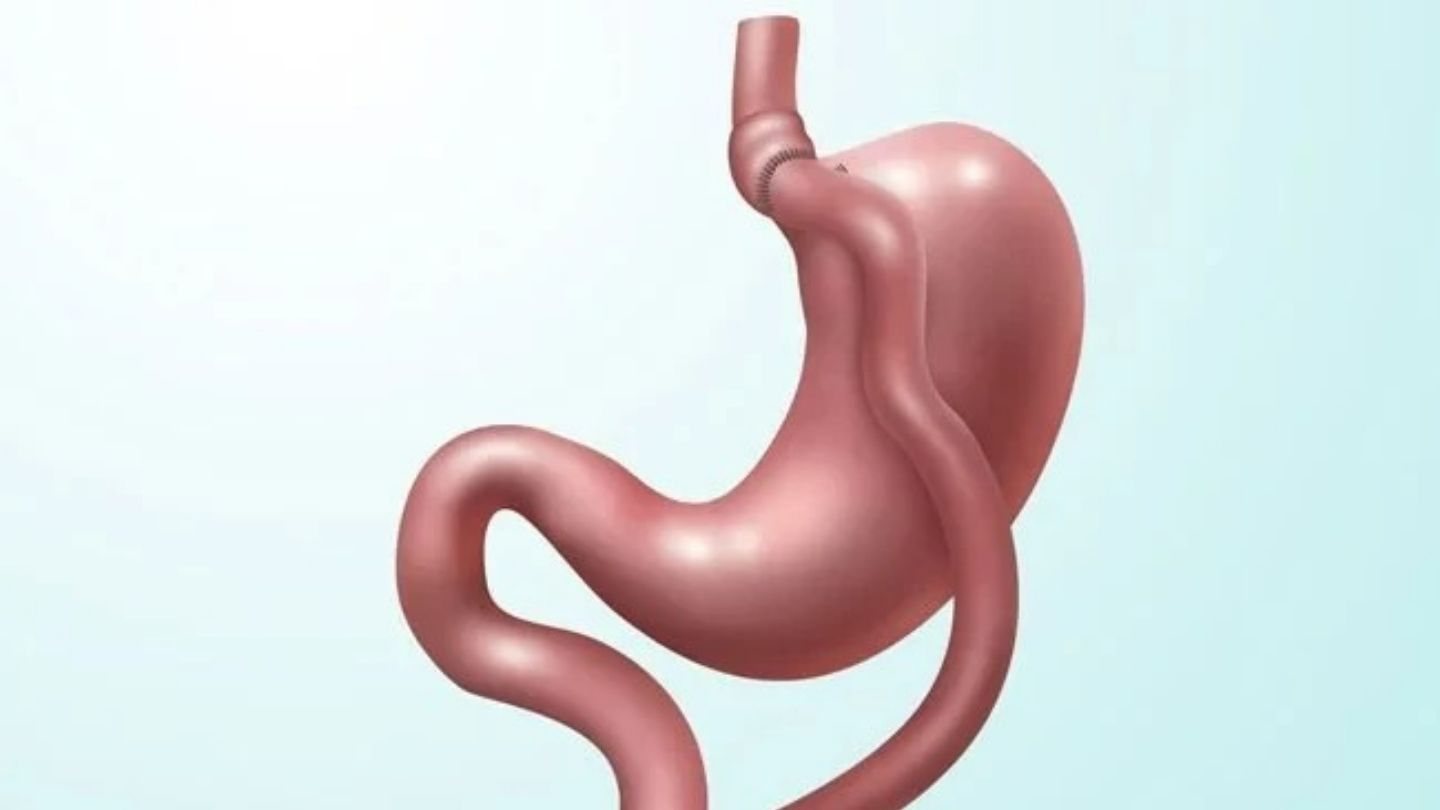
What BMI Is Required for Gastric Sleeve Surgery?
If you’re exploring weight loss surgery as a path to better health, you’re likely wondering about the specific requirements that determine candidacy. Understanding what BMI is required for gastric sleeve surgery helps you know where you stand and what steps come next. This blog walks through the standard criteria, exceptions, and everything else that factors into becoming a good candidate for this life-changing procedure.
Key Takeaways
- Most adults qualify for gastric sleeve surgery at a BMI of 40 or higher, or at a BMI of 35–39.9 when accompanied by serious obesity-related health problems such as type 2 diabetes, severe sleep apnea, or high blood pressure.
- Some bariatric centers may consider patients with a BMI of 30–34.9 if they have uncontrolled metabolic diseases and other weight loss methods have not worked, though this depends on local guidelines and insurance coverage.
- BMI is only one part of the evaluation process; your medical history, mental health readiness, and commitment to permanent lifestyle changes are equally important.
- Only a bariatric surgeon or specialist can confirm your individual eligibility after completing a full assessment tailored to your unique health situation.
Understanding BMI and How It’s Calculated
Body mass index, commonly called BMI, serves as the primary screening tool that healthcare providers use to assess eligibility for gastric sleeve surgery. This measurement offers a standardized way to evaluate whether someone falls into categories that indicate severe obesity and its associated health risks.
BMI is calculated using a straightforward formula: your weight in kilograms divided by your height in meters squared. For example, an adult who weighs 120 kg and stands 1.7 meters tall would have a BMI of approximately 41.5—placing them in the highest obesity category. Here’s how the standard adult BMI categories break down:
- Underweight: Below 18.5
- Normal weight: 18.5–24.9
- Overweight: 25–29.9
- Class I obesity: 30–34.9
- Class II obesity: 35–39.9
- Class III (severe) obesity: 40 and above
It’s important to understand that body mass index BMI functions as a screening tool rather than a perfect measure of health. The calculation can overestimate body fat in very muscular individuals—such as competitive athletes—and may underestimate it in certain ethnic groups or older adults with reduced muscle mass. For adolescents and children, BMI interpretation uses age- and sex-specific growth charts rather than these fixed adult cutoffs, recognizing that young bodies are still developing. In a comprehensive guide to gastric sleeve surgery, BMI is often used as one of the primary criteria to determine eligibility and assess potential benefits of weight-loss treatment.
Minimum BMI for Gastric Sleeve in Adults
The most straightforward answer to the question of BMI requirements comes from guidelines established by the American Society for Metabolic and Bariatric Surgery (ASMBS) and supported by decades of research since the original 1991 NIH consensus standards.
For most adults, gastric sleeve surgery, also known as sleeve gastrectomy or vertical sleeve gastrectomy, becomes an option under these criteria:
BMI of 40 or higher: Adults with class III obesity typically qualify regardless of whether they have additional health conditions, provided they have attempted supervised weight loss without achieving lasting results.
BMI between 35 and 39.9 with comorbidities: Adults in this range may qualify when they have at least one serious obesity-related condition. Common qualifying conditions include:
- Type 2 diabetes
- Severe sleep apnea documented by a sleep study
- Hypertension (high blood pressure)
- Heart disease
- Nonalcoholic steatohepatitis (NASH)
BMI between 30 and 34.9 with metabolic disease: Updated guidelines from the ASMBS now extend consideration to adults with lower BMI who have poorly controlled type 2 diabetes or metabolic syndrome when diet and exercise habits and medications have failed to produce adequate results.
Beyond BMI, certain factors can exclude otherwise eligible patients. These include active substance abuse, uncontrolled psychiatric illness, or an inability to commit to the long-term follow-up and lifestyle changes that metabolic and bariatric surgery requires.
BMI Requirements for Gastric Sleeve in Adolescents

When it comes to teenagers, eligibility criteria become significantly more stringent. Any adolescent being considered for bariatric surgery will be evaluated by a specialized multidisciplinary team that includes pediatric surgeons, dietitians, behavioral health specialists, and other experts in adolescent medicine.
The typical BMI thresholds for teens use percentile-based measurements rather than fixed numbers:
- BMI at or above 120% of the 95th percentile for age and sex (roughly equivalent to an adult BMI of 35) qualifies when accompanied by major comorbidities such as type 2 diabetes, hypertension, or nonalcoholic fatty liver disease.
- BMI at or above 140% of the 95th percentile (roughly equivalent to an adult BMI of 40) may qualify even without documented comorbidities.
Beyond the numbers, healthcare teams consider puberty stage (typically Tanner stage 2 or higher), skeletal maturity, emotional readiness, and the level of family involvement and support. Most guidelines require that non-surgical treatments—including structured diet programs, increased physical activity, and behavioral therapy—have been attempted for at least 6 to 12 months without producing sufficient weight loss.
Not every bariatric center performs procedures on adolescents. Families pursuing this option may need referral to specialized pediatric bariatric programs with experience in this population.
Health Conditions That Influence BMI Eligibility
Obesity-related health problems can make gastric sleeve surgery medically necessary at a lower BMI than the standard 40 threshold. These conditions demonstrate that excess weight is actively harming your body and that surgical intervention offers meaningful benefits beyond weight loss alone.
Key conditions that often justify surgery at BMI 35–39.9 (or even 30–34.9 in some protocols) include:
- Type 2 diabetes: Particularly when medications like metformin or GLP-1 agonists combined with lifestyle changes fail to adequately control blood sugar levels
- Moderate to severe obstructive sleep apnea: Documented through polysomnography (sleep study), especially with an apnea-hypopnea index above 30
- Resistant high blood pressure: Blood pressure remaining above 140/90 mmHg despite taking three or more medications
- Heart disease: Including established cardiovascular conditions or significant risk factors
- Nonalcoholic fatty liver disease or NASH: Particularly when liver biopsy or elastography shows fibrosis
- Severe joint disease: Mobility-limiting osteoarthritis of the hips or knees that significantly impacts quality of life
- Breathing problems: Including obesity hypoventilation syndrome
Documentation of these conditions through appropriate blood tests, imaging studies, and specialist evaluations is typically required for insurance preauthorization. Without proper documentation, claims may be denied.
It’s worth noting that some conditions may actually steer the recommendation toward a different procedure. For example, severe gastroesophageal reflux disease (GERD) can worsen after a gastric sleeve, leading many surgeons to recommend gastric bypass surgery instead for patients with significant reflux. This consideration is often discussed alongside the role of ghrelin in weight loss after gastric sleeve surgery, since hormonal changes can also influence how patients respond to different bariatric procedures.
Improving or preventing progression of these obesity-related conditions represents a primary goal of metabolic surgery—the benefits extend well beyond the number on the scale.
Other Factors Beyond BMI in Gastric Sleeve Candidacy
While BMI provides an important starting point, eligibility for stomach sleeve surgery involves a comprehensive evaluation that examines your complete health picture and readiness for permanent change.
Non-BMI Eligibility Requirements
- Documented weight loss attempts: Most programs and insurers require evidence that you’ve tried supervised weight loss through other methods for 6 to 12 months without achieving lasting success. This typically means working with a dietitian, primary care doctor, or structured weight management program with regular weigh-ins.
- Age considerations: The commonly accepted age range runs from 18 to 65, though some centers extend this to 70 or beyond for patients who are otherwise healthy and have low surgical risk.
- Psychological readiness: Candidates must demonstrate emotional stability and the absence of uncontrolled eating disorders such as active bulimia, severe untreated depression, or other psychiatric conditions that could interfere with recovery and adherence to post-surgical protocols.
Preoperative Assessment Components
Before proceeding with laparoscopic surgery, your team will typically complete a series of evaluations that also help you understand how long gastric sleeve surgery takes and what the full timeline looks like:
- Nutrition consultation: A registered dietitian reviews your eating habits, identifies nutritional deficiencies, and begins education about post-surgical eating patterns
- Psychological evaluation: A behavioral health specialist assesses your expectations, coping mechanisms, and support systems
- Medical testing: Blood work including hemoglobin A1c and lipid panels, ECG to check heart function, and possibly abdominal imaging, upper endoscopy, or sleep studies, depending on your individual risk factors
Lifestyle Commitment
Long-term success with the gastric sleeve requires permanent changes. You’ll need to commit to:
- Following a high-protein diet (60–80 grams daily)
- Engaging in regular exercise (approximately 150 minutes weekly)
- Taking daily multivitamins and supplements to prevent deficiencies
- Attending follow-up appointments for years after surgery
- Portion control and mindful eating patterns
Insurance companies may add their own requirements, such as mandatory nutrition classes, psychological clearance letters, or specific documentation periods before approval.
What If Your BMI Is Below the Standard Threshold?
If your BMI falls below 35 but you’re still struggling with your weight and related health problems, you may feel uncertain about whether bariatric surgery is an option. The good news is that eligibility criteria have evolved in recent years.
Options for BMI 30–34.9
Some specialized centers and newer guidelines now permit gastric sleeve surgery for adults with a BMI between 30 and 34.9 when:
- Type 2 diabetes or metabolic syndrome remains poorly controlled despite appropriate medications
- Multiple weight loss procedures and programs have failed despite genuine effort and adherence
- The individual fully understands the lifelong implications, necessary lifestyle modifications, and potential risks
Research, including data from studies like STAMPEDE, has demonstrated that patients in this BMI range can achieve significant weight loss and diabetes remission rates comparable to those with higher BMI.
Options for BMI Below 30
For adults with a BMI under 30, a gastric sleeve is rarely indicated and almost never covered by insurance. In exceptional circumstances, some individuals may access surgery through clinical trials exploring metabolic interventions for lower-BMI patients with diabetes.
If you’re below standard thresholds, consider:
- Intensive medical weight management: Newer medications like tirzepatide and semaglutide can help you lose weight significantly—some patients see 15–22% body weight reduction
- Clinical trial participation: Ask your healthcare team about ongoing research studies in your area
- Comprehensive lifestyle assessment: Review whether medication side effects, underlying medical conditions, or other factors might be contributing to weight challenges
Every case is individualized. The final decision rests with your bariatric team after a thorough evaluation—not solely on a BMI number.
Preparing for Gastric Sleeve Once You Meet BMI Criteria

Meeting BMI requirements opens the door to surgery, but the journey doesn’t end there. A preparation period helps ensure the best possible outcomes and gives you time to build habits that support long-term weight loss.
Pre-Surgery Steps
- Education: Most programs require attendance at bariatric education classes or seminars. These sessions explain what happens during the procedure, outline risks such as blood clots or staple-line complications, and help you understand the digestive system changes you’ll experience.
- Pre-operative diet: You’ll typically follow a liver-shrinking diet for 1–2 weeks before surgery. This usually involves 800–1,200 calories daily with high protein and very low carbohydrates (under 40 grams), which reduces liver size by approximately 30% and makes laparoscopic surgery safer.
- Smoking cessation: If you smoke, you’ll need to stop at least 4–8 weeks before surgery. Quitting reduces complication risk by roughly 50% and supports better healing.
Medical Testing
Your doctor will order various tests before clearing you for general anesthesia:
- Complete blood tests, including liver function and nutritional markers
- ECG and possibly echocardiogram for patients with very high BMI or cardiac risk factors
- Chest X-ray
- H. pylori testing (a bacterium that can cause stomach problems)
- Upper endoscopy to examine the upper belly and digestive tract
- Sleep study if obstructive sleep apnea hasn’t been previously evaluated
Planning for Recovery
Success requires planning beyond the hospital and learning what to expect during gastric sleeve recovery time after surgery:
- Arrange help at home during the first weeks of recovery
- Plan for time off work (typically 2–4 weeks depending on your job)
- Stock your kitchen with appropriate soft foods and pureed foods for the early post-surgical diet, following guidance that can also help manage nausea after gastric sleeve surgery and promote comfort
- Schedule follow-up visits and lab checks in advance
- Connect with support resources, whether through your bariatric program or online communities
Setting Realistic Expectations
Patients who undergo a gastric sleeve typically lose 50–70% of their excess body weight within 12–18 months. However, results vary based on adherence to diet and exercise recommendations, metabolic factors, and individual biology. Regular follow-up with your multidisciplinary team helps monitor nutritional status, address challenges, and support lifestyle adjustments that prevent you from regaining weight over time.
Understanding Eligibility for Bariatric Surgery
BMI plays an important role in determining eligibility for gastric sleeve surgery, but it is not the only factor doctors consider. Overall health, obesity-related conditions, and previous weight-loss efforts also influence candidacy. Consulting with a qualified medical team helps ensure patients receive the safest and most appropriate treatment plan for long-term weight management success.
Wellstar Comprehensive Bariatric Services offers expert guidance for individuals considering the gastric sleeve in Austell, Marietta, Smyrna, Cobb, LaGrange, and West GA, helping patients understand eligibility requirements and available treatment options. Our team also provides specialized care for GERD, lap band correction, and gastric bypass procedures. Contact us today to learn more about your options and begin your journey toward improved health.
Frequently Asked Questions
Can I get gastric sleeve surgery if my BMI is under 35 but I have severe diabetes?
In some centers and under certain international guidelines, adults with BMI 30–34.9 and poorly controlled type 2 diabetes may be considered for metabolic surgery when medications and lifestyle measures have failed. The American College of Surgeons and ASMBS have expanded recommendations to include this population based on evidence showing excellent diabetes remission rates. However, acceptance depends heavily on local regulations, your surgeon’s specific policies, and insurance coverage. Discuss your situation directly with a bariatric team to understand your weight loss options.
Is there a maximum BMI for gastric sleeve surgery?
There’s generally no absolute upper BMI limit, but patients who are severely overweight with very high BMI (approximately 60 or above) face increased surgical risks, including complications during general anesthesia. Many centers recommend staged treatment for super-obese patients—this might include initial weight loss through medical management or a different procedure like gastric banding before proceeding to sleeve gastrectomy. Some facilities also have equipment limitations; for example, imaging tables may have weight limits of around 450 pounds.
How long do I need to try diet and exercise before qualifying for surgery?
Many programs and insurers require documented supervised weight-loss attempts over 6–12 months before approving bariatric surgery. This typically includes regular visits with a dietitian, your primary care medicine provider, or participation in a structured weight management program with weights recorded at each appointment. The purpose is to demonstrate that conservative approaches haven’t produced adequate results and to help you build exercise habits that will support post-surgical success.
Does my BMI requirement change if I choose gastric bypass instead of gastric sleeve?
BMI thresholds for gastric bypass surgery and gastric sleeve are generally the same, as guidelines focus on the presence of severe obesity and related health risks rather than the specific procedure. The choice between procedures depends more on individual factors such as the severity of reflux disease (bypass may be preferred for severe GERD), diabetes control goals, and your surgeon’s recommendation based on your anatomy and health history.
Will losing weight before surgery lower my BMI too much to qualify?
This concern comes up often, but modest pre-surgery weight loss required by your team won’t typically affect eligibility. Surgeons document your baseline BMI at the initial assessment for insurance and guideline purposes. The 2-week liver-shrinking diet and any weight loss during the evaluation period are viewed as improving safety and surgical outcomes—not as reasons to disqualify you. In fact, demonstrating commitment to small cuts in calories and improved eating habits before surgery often predicts better long-term success after the procedure.